The Tibialis Muscles & Lower Limb Injury Risk: What You Need to Know

Hunter Bennett
Hamstring and Achilles injuries are some of the most common to plague track and field athletes alike. Both play an integral role in the force production processes of the posterior chain, allow the transfer of force from the hip right down into the foot. With this in mind, their effective function is integral to the successful performance of high force and high-velocity movements, such as sprinting, jumping, and bounding.
As such, preventing injuries within these areas is essential. Unfortunately, most people take a somewhat one-dimensional approach to injury prevention, in which they strictly focus on increasing the strength and capacity of the individual muscle group in question. Now while this is certainly a piece of the injury prevention puzzle – it is simply that, a single piece of a much larger puzzle. Which is why looking at the rest of the leg and how to interacts with the rest of the limb can be an absolute game changer (Neal, 2014). Particularly the shank, with emphasis on the tibialis muscles: tibialis anterior, and tibialis posterior.
The Tibialis Muscles
As previously mentioned, the tibialis muscle group can be separated into two distinct muscles – the tibialis anterior and the tibialis posterior.
Tibialis Anterior
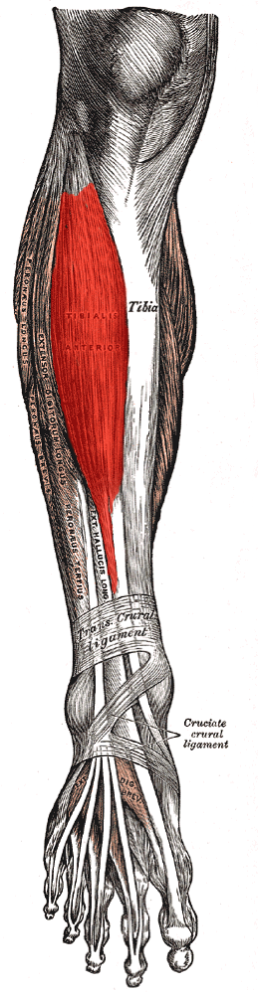
The tibialis anterior muscle sits right in the middle of the anterior compartment of the lower leg. Its primary role in a purely anatomical sense is to dorsiflex and invert the foot. In a more functional sense, tibialis anterior plays an important role in the force transfer of the lower limb by providing stability to the shank during walking, running, jumping, and bounding (Munoz, 2015). You see, it acts to stabilize the ankle as the foot hits the ground during the contact phase of these movements, and then proceeds to pull the foot clear of the ground during the swing phase of these same movements.
Source: https://commons.wikimedia.org/wiki/File:Tibialis_anterior_2.png
Related Article: Is Quality Sleep a Predictor for Sports Injury?
Tibialis Posterior
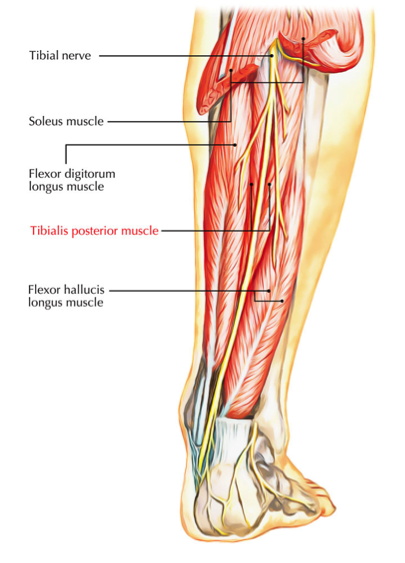
Acting as the primary antagonist to tibialis anterior, the tibialis posterior muscle sits within the posterior portion of the calf. As such, its anatomical functions include inverting the foot and ankle and facilitating plantar flexion of the ankle.
However, much like the tibialis anterior, its primary functional role is to provide stability to the lower leg during athletic movements. Moreover, this key muscle also provides much-needed support to the foot’s medial arch, in which it is essential to maintaining a firm foot during those same athletic movements. (Maharai, 2016) As a result, it is integral to maximizing force production during acceleration, jumping, bounding, and when running at maximal velocity.
Source: https://www.earthslab.com/anatomy/tibialis-posterior/
Tibialis and Injury Causes
Now, if either the tibialis anterior or posterior (or both, for that matter) are not functioning correctly and are therefore incapable of stabilizing the lower limb, then we are going to have some serious issues. More specifically, when the foot strikes the ground during athletic movement tasks, the lower leg and talus will glide forward on the other tarsal bones. With this glide, you can also expect to see excessive pronation of the foot, combined with excessive inversion of the ankle. Not pretty.
In the most immediate sense, this is going to place the ankle in an undesirable position, potentially opening it up to an increased risk of inversion sprain – particularly in those individuals who participate in field sports that involve jumping and bounding on somewhat uneven surfaces such as grass. But this can also cause some issues in a more chronic manner – relating to both the Achilles and the Hamstrings.
Tibialis Muscles and Achilles Injury
Because both tibialis muscles are not doing their job effectively, the muscles of the posterior chain must act as stabilizers as well as prime movers during these specific movement tasks. This increase in load can contribute to a rapid increase in stiffness of the Achilles (and often the plantar fascia it connects to) as means to help stabilize the lower limb and ankle and restrict this unwanted and excessive movement. While beneficial in the short term, this potent combination of increased loading and stiffness actually overloads the Achilles tendon. This increases the risk of tendinopathy occurring, while also reducing its force transfer capacity.
The result is an increased risk of injury, combined with a reduction in power output.
Source: http://austinsportstherapy.com/injury-prevention/the-posterior-chain-its-all-in-the-hips
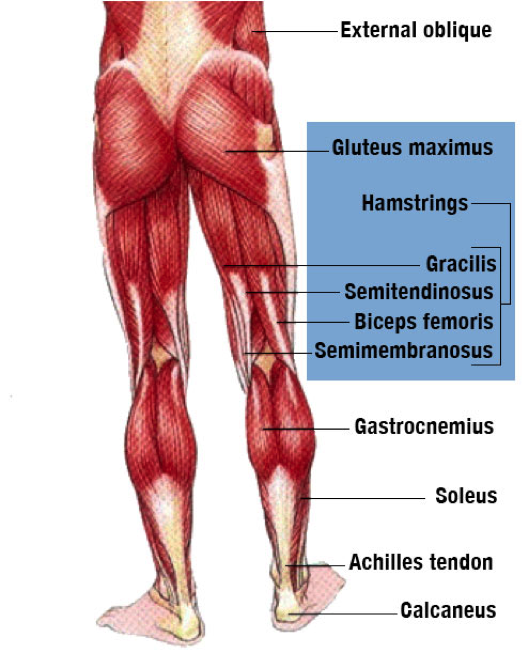
Tibialis Muscles and Hamstring Injury
In a very similar manner to the above, this loss of stability and increase in eversion causes some issues up the kinetic chain – one of which is the exacerbation of internal rotation during the contact phase of gait. To try and mitigate this excessive internal rotation and limit the inversion occurring at the ankle, the lateral most hamstring muscle (the bicep femoris, for you nerds out there) increases its stiffness to restrict this undesired movement. In this manner, it begins to act again as a stabilizer and a primary hip extensor during movement. And very similar to the Achilles, this rapid increase in load can seriously increase the risk of developing a lateral hamstring tendinopathy, while also inhibiting force production. Now where we see a further issue is that this also contributes to the shortening of the muscle group, which can increase its risk of a strain or tear – which is obviously pretty damn undesirable.
What are the Signs of Injury?
So first and foremost, we can have a quick look at the areas of injury and see if the signs line up. While I wouldn’t recommend this as a purely diagnostic tool, it can give you some insight into whether your tibialis musculature is functioning effectively or not.
What are the signs of Achilles Injury?
There are certain signs you can look for with an Achilles injury caused by tibialis dysfunction. These include:
- Sensations of pain and stiffness within the tendon.
- The worsening of pain when the tendon is placed under load.
- Increases in pain and stiffness during the night or when you first wake up.
- The tendon may be tender, swollen, and ‘rough’ to touch.
- You notice a ‘crunchy’ feeling when loading the tendon.
What are the signs of Hamstring Injury?
Much like the Achilles tendon, there are specific signs that you can look for with a hamstring injury caused by declines in tibialis function. These include:
- Sensations of pain and stiffness throughout the lateral hamstring.
- Sensations of pain in the lateral portion of the high hamstring attachment, which worsens when sitting.
- The worsening of pain when the hamstring is placed under load or stretch.
- The high tendon may be tender, swollen, and ‘rough’ to touch.
- A significant loss of hamstring flexibility on the affected side.
What are the signs of Tibialis Dysfunction?
And finally, we can also help identify if your tibialis muscles are contributing to the problem by looking at the feet to identify some signs of tibialis dysfunction. These include:
- A flat, or overly pronated foot.
- A heavily inverted ankle.
- External rotation of the foot, with the toes pointing out slightly.
- Limited ankle dorsiflexion range of motion.
- Tightness identified through the plantar fascia when rolling the bottom of the foot with a lacrosse ball or golf ball.
Related Article: Injured? Increase Your Muscle Mass with Blood Flow Restriction Training
Injury Treatment: The Tibialis Fix
Now, there are a couple of stages of correcting these observed dysfunctions as a way to reduce injury risk ad enhance performance.
Firstly, we want to reduce any unnecessary tension through the posterior chain. This means foam-rolling your calves, lateral hamstring, adductors (which share a fascia train with tibialis posterior), and your glutes, while also getting into the plantar fascia and tibialis posterior with a lacrosse ball. Prepare for some ‘slight’ discomfort. Once we have released tension through the posterior chain and restored the tibialis muscles capacity to function, its time to strengthen up those muscles in a functional manner (Kelly, 2013). Which is where the following three exercises come into play.
The 3 Best Tibialis Exercises
These three exercises provide the ideal method of enhancing the strength of these key muscles in a manner that replicates their function in athletic tasks. As a result, they can improve their ability to tolerate load and stabilize the lower limb, while also causing vast increases in the ability for the feet to transfer force – thus increasing performance and reducing injury risk.
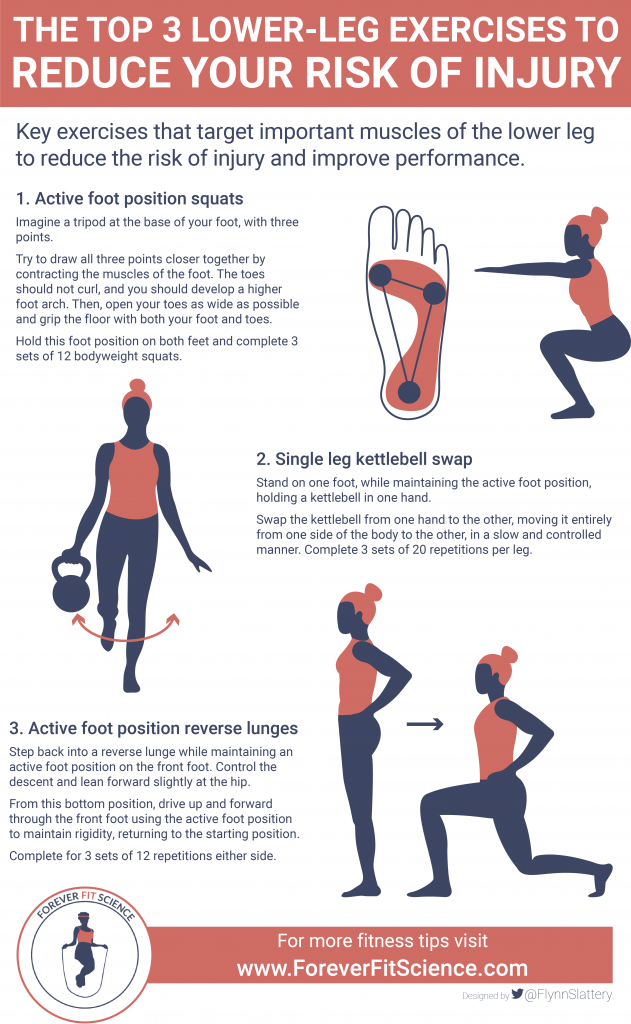
Active Foot Position Squats
Our first step is to teach what is known as ‘an active foot position’ to get these muscles working effectively to stabilize the foot and ankle.
- Our first step is to imagine that you have a tripod at the base of your foot. In this manner, one point is under the big toe section of the ball of your foot, another under the lateral section of the ball of your foot, and the last is under the heel.
- Once you can actively feel these three points, draw all three points closer together by contracting the muscles of the foot. The toes should not curl, and you should develop a higher foot arch.
- Once you feel comfortable with this solid position, proceed to open your toes as wide as possible and grip the floor with both your foot and toes. Your foot should feel like it’s holding a plank.
- Now finally try to hold this foot position on both feet and complete some bodyweight squats. 3 sets of 12 should do the trick.
Single Leg Kettlebell Swap
Popularised by Dr. Joel Seedman of Advanced Human Performance, this great exercise reinforces the active foot position mentioned above in a way that further enhances strength and stability.
- First thing is to get into the active foot position we developed in the previous exercise while holding a kettlebell in one hand.
- Proceed to stand on one foot, without losing that foot position.
- The final step is to swap the kettlebell from one hand to the other, moving it entirely from one side of the body to the other, in a slow and controlled manner. Complete 3 sets of 20 repetitions per leg.
Active Foot Position Reverse Lunges
Now with this final exercise, you are going to be reinforcing the active foot position used above in a highly dynamic, and single leg, manner. This replicates the demand placed on these muscles in the athletic movement tasks we have mentioned above, directly enhancing functional capacity.
- First thing is to get into the active foot position we developed in the previous exercise.
- Proceed to step back into a reverse lunge, controlling the descent and leaning forward slightly at the hip – all whilst maintaining the active foot position on the front foot.
- From this bottom position, drive up and forward through the front foot using the active foot position to maintain rigidity, returning to the starting position.
- Complete for 3 sets of 12 repetitions either side.
Take Home Message
The tibialis muscles are integral to proper foot and ankle function. They provide stability to the foot, ankle, and lower limb, reducing injury risk and allowing proper force transfer. Unfortunately, they are often overlooked in injury prevention programs.
With this in mind, when they are functioning poorly, the Achilles and hamstring are forced to act as stabilizers, which can reduce their functional capacity and increase injury risk.
But by implementing the tips outlined in this article, you can restore foot and ankle function, reduce your risk of injury, and enhance performance in a big way!
References
Neal, Bradley S., et al. “Foot posture as a risk factor for lower limb overuse injury: a systematic review and meta-analysis.” Journal of foot and ankle research 7.1 (2014): 55.
Munoz, Maria Ruiz, Manuel González-Sánchez, and Antonio I. Cuesta-Vargas. “Tibialis anterior analysis from functional and architectural perspective during isometric foot dorsiflexion: a cross-sectional study of repeated measures.” Journal of foot and ankle research 8.1 (2015): 74.
Maharaj, Jayishni N., Andrew G. Cresswell, and Glen A. Lichtwark. “The mechanical function of the tibialis posterior muscle and its tendon during locomotion.” Journal of biomechanics 49.14 (2016): 3238-3243.
Kelly, Luke A., et al. “Intrinsic foot muscles have the capacity to control deformation of the longitudinal arch.” Journal of The Royal Society Interface 11.93 (2014): 20131188.
You Might Like: