Exercise and Sleep Disorders — Sleep Series Part 5

Gillian White, MSc., PhD (Candidate), University of Toronto, Graduate Department of Exercise Sciences
Sleep Stats And General Information – Sleep Series Part 1
Sleep Physiology – Sleep Series Part 2
Sleep And Health – Sleep Series Part 3
Exercise And Sleep Quality – Sleep Series Part 4
1. Sleep Apnea
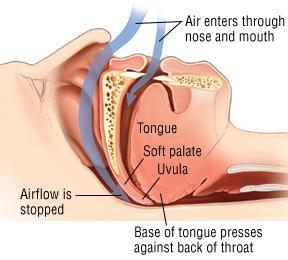
Figure 1. Deformation of airways causing obstructive sleep apnea.
What Is Sleep Apnea?
Sleep apnea is one of many sleep disorders and can be either obstructive (shown in figure 1) – a physical deformation of airways causing obstruction – or central, in which your brain “forgets” to send signals to your lungs to breathe. In either case, it results in you stopping breathing briefly a few times an hour during sleep. This impairs oxygen uptake in the blood and reduces the efficacy of a number of active sleep processes (immune activation, repair etc.) and impairs your ability to get into a deep sleep.
Overall, you’re left with the characteristics of poor sleep – poor attention and focus, lower working memory and learning, irritability and poor self-control, and overall sleepiness. These functional changes relate to structural changes in the brain, especially in the hippocampus and frontal cortex (Canessa et al. 2010). Because it disturbs the important processes of sleep that are critical to maintaining good heath, it is also associated with higher risk of heart disease & stroke, diabetes & obesity, and accidents.
Who Is Affected By Sleep Apnea?
Obstructive sleep apnea is defined as 5 or more events (breathing stops) per hour during the night and affects more than 25 million Americans (Institute of Medicine, 2006). Typically, you’ll only know if you have sleep apnea if someone tells you or if you do a sleep study, but if you feel chronically unrested you may want to investigate with your doctor. It effects more males than females, and is also more prevalent in smokers, drinkers, and people who are sedentary and/or overweight. Therefore, lifestyle factors can have a very big impact on the progression and severity of sleep apnea.
How Does Exercise Help?
Often people with sleep apnea will use a Darth Vader-like CPAP machine that uses pressurized & oxygenated air to help maintain breathing and O2 levels throughout the night. These machines are cumbersome (and a bit scary looking) and inconvenient, and may not treat the underlying cause of sleep apnea, which is thought to be related to systemic inflammation or autonomic dysregulation (Dempsey, 2010). Other lifestyle changes that improve inflammation including weight loss, smoking/drinking cessation, and exercise can help. Excess weight is a particularly impactful risk factor, so reducing excess body weight through diet and exercise can be very effective in reducing sleep apnea symptoms. Exercise also promotes an autonomic shift and anti-inflammatory effect, which likely contribute to its effect on sleep apnea.
Related Article: Exercise Induced Sleep Improvements
Research/Evidence
Like many other conditions for which exercise is a sort of treatment, some of the evidence comes from epidemiological self-reports, which have found that people who are physically active have a lower risk of sleep apnea (Kline et al. 2011). Exercise participation (150min/week) is associated with lower AHI events per night, the scale used to measure apnea severity. Further, sleep quality and blood oxygenation have been found to be related to changes in physical fitness (Kline et al. 2011).
Exercise independently improves many of the cognitive and structural changes that are characteristic of sleep apnea, as it is known to promote hippocampal growth and function (Erickson et al. 2010), learning and memory (Deng, Aimone, & Gage 2010), executive functioning, and mood/self-regulatory processes (Goldin et al. 2013). A more detailed description of exercise and sleep apnea can be found in the article here.
2. Insomnia
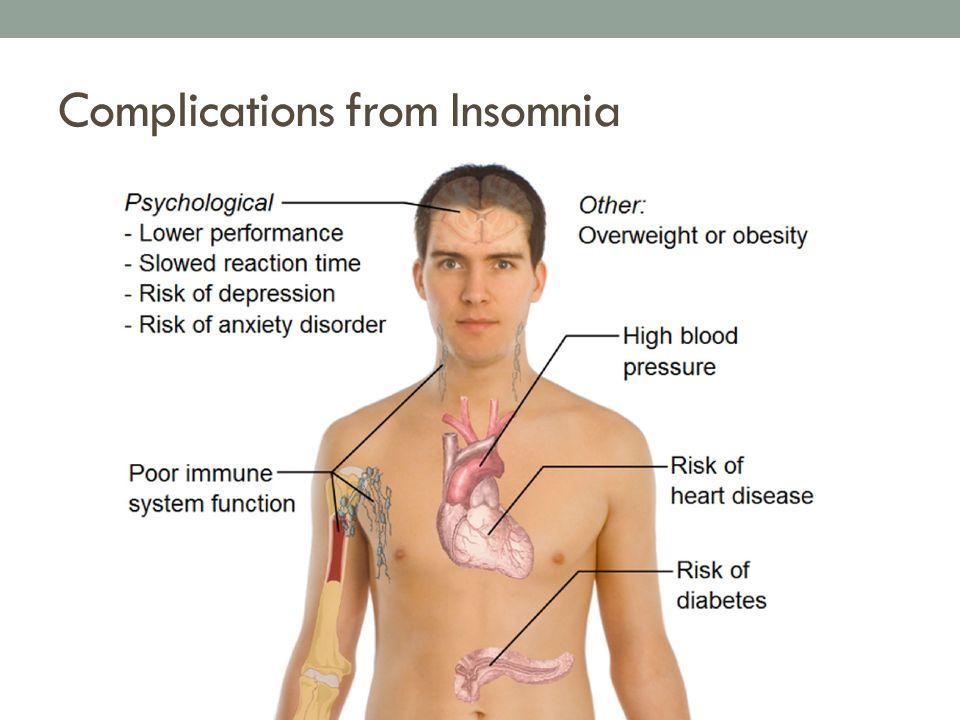
Figure 2. Complications of insomnia.
What Is Insomnia?
Insomnia is a well-known affliction that refers to significant loss of sleep – either getting to sleep or staying asleep, or non-restorative sleep. It results in loss of function during the day and other negative consequences of impaired sleep (mental/physical health, performance, cognitive function, mood emotional regulation etc.). There is no explicit cure for insomnia, so sleep habits and/or lifestyle changes are the first line of defence for improving insomnia episodes. As its origin is largely psychological, it is often the result of other underlying conditions like stress, depression/anxiety, chronic pain, etc. or lifestyle habits like alcohol, caffeine, or smoking. However, in some cases it is considered “primary” insomnia with no underlying causes.
Who Is Affected By Insomnia?
Insomnia affects about 10-15% of adults and is more common in females than males, and in older people compared to younger. About 6% of the population experiences insomnia that is not related to some underlying cause of sleep disturbance (primary insomnia). In addition to consistent sleep loss (>3 nights/week for >3 months), dysfunction to social, occupational, educational, academic, or behavioral ability is also required for a clinical psychiatric diagnosis of insomnia.
How Does Exercise Help?
Sleep aides (i.e. pills) can be addictive or lose efficacy over time. They can only be used as a band-aid solution. One characteristic of people suffering from insomnia is increased urinary cortisol and catecholamines (HPA/SNS activation) and higher brain and body energy use (especially glucose). Overall, this points to chronic and excessive arousal of both the brain and body’s systems. This makes it difficult to turn them down enough to get effective rest (deep sleep). This can possibly result from altered neurotransmitter populations, specifically GABA an important inhibitory neurotransmitter.
Ultimately, it results in a cycle in which you can’t sleep, which impairs your body and brains ability to fully relax and repair, which causes greater activation of your body further worsening sleep issues and so on. Exercise can help promote the shift towards relaxation interrupting this dysfunction sleep cycle and starting you on a path to better sleep.
Research/Evidence
Exercise early in the day helps decrease stress and psychological influences of insomnia. This happens because of a shift in the autonomic nervous system balance towards parasympathetic activity. This decreases basal activation of fight/flight signaling molecules (catecholamines and cortisol). Furthermore, it normalizes GABA concentration and activity in the brain. Overall, it means your body’s baseline is more relaxed. Acute exercise (i.e. exercise this morning) can improve insomnia so long as the timing is not close to bed time, given the physiologically arousing effects of exercise. Moderate intensity aerobic exercise seems to be better than resistance training and aerobic combined, or high-intensity exercise for alleviating the severity of insomnia symptoms (Passos et al. 2010).
Exercise training programs have also shown great improvements in insomnia symptoms, regardless of time of day exercise is done (slightly different than the results of one-off exercise bouts and insomnia symptoms). Participants (~45 years old) in an exercise trial fell asleep in ~8 min compared with 17 min, woke up in the night for 40 minutes compared with over an hour, improved sleep quality from 41% to 60%, and felt significantly better rested in the morning (Passos et al. 2011). Similar findings have also been found in older individuals with chronic insomnia (>55 years old) (Reid et al. 2010). These findings suggest improvements in sleep are related to improvements in psychological functioning.
Related Article: 4 Tips For Balancing Sleep & Exercise
3. Bruxism
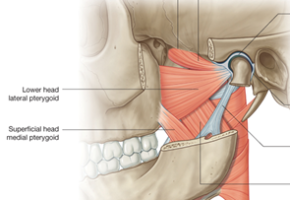
Figure 3. Jaw muscle activation leading to one of many sleep disorders: bruxism.
What Is Bruxism?
Bruxism essentially refers to teeth grinding or jaw clenching during sleep. Hence, symptoms tend to be worse during the day (headaches, tooth soreness) but the cause is clenching/grinding at night. However, often you don’t notice it but you carry a lot of tension in your jaw muscles. Ultimately, this can result in dental issues (sensitive/filed down teeth), tension headaches, or jaw issues.
Who Is Affected By Bruxism?
70% of the underlying cause of bruxism relates to stress and seems to be worse for people who sleep on their back. Usually during sleep, because the paralysis of skeletal muscles that occurs, the voluntary muscles of the jaw are inactive and the jaw relaxes and opens slightly. Over-arousal of muscles – possibly because of neurotransmitters, or heightened sympathetic activation – causes clenching or grinding of the jaw. There are no real demographic risks for bruxism but people at risk of physiological stress – i.e. people with anxiety, low levels of physical activity, high stress occupational or personal lives – may have a higher risk.
How Does Exercise Help?
Aides for bruxism include mouth guards, pharmaceuticals to treat the possible underlying neurological causes, psychosocial stress coping, and muscle relaxants/paralyzers (Botox). In general, the treatment either has to protect the teeth, relax the jaw muscles, or treat the underlying stress that is causing the over-activation. And it is this over-activation that causes tensing of muscles during sleep. Exercise can promote the latter two. It reduces muscle activation with a compensatory shift from sympathetic activation to parasympathetic activation. In turn, this reduces psychological stress, anxiety, and worry. Furthermore, it reduces the somatic (body) manifestation of stress.
Research/Evidence
There isn’t any peer-reviewed research investigating the effects of exercise on bruxism. However, given the contribution of psychological stress to its occurrence, there’s a strong likelihood that exercise and relaxation can help manage the causes and the symptoms of it. With this in mind, the best exercise is probably aerobic or HIIT. This is because these exercises have strong anti-stress and anti-anxiety effects. Also, yoga/mindfulness practices can help promote better control over muscle activation and reduce that baseline state of being “keyed-up” that comes with too much stress.
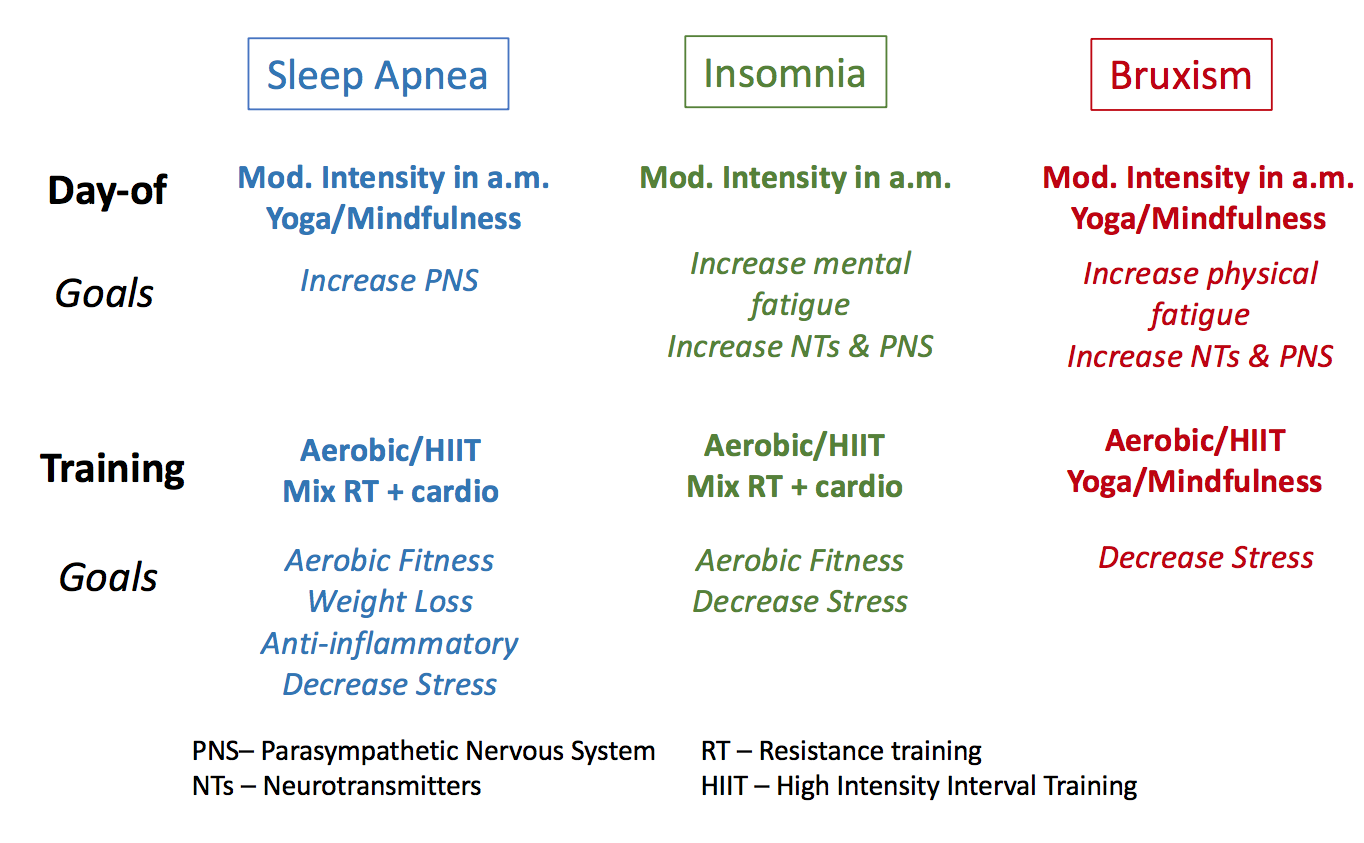
Figure 4. Evidence-based exercise strategies for short term (day-of) and long-term (training) effects on sleep disorders.
Parting Thoughts:
We’re busy, productive, successful people. We have a lot on the go and sometimes fitting everything into a day can be challenging. For people like us, it is critical to keep the wide-ranging health and function effects of sleep in mind. Functionally, we can choose to make time to do a hundred things at 70% of our potential. Or, we can choose to do fewer things at 100% of our potential. Investing in sleep is not only investing in how your brain and body feel day to day, but how they’ll feel and function over your lifetime.
Get to sleep an hour before midnight. Turn off electronics 30 minutes before bed. Exercise in the morning to promote an early night’s sleep and a deep, restorative sleep. All of this can lead us to be the best version of ourselves, without sacrificing health or sanity in the process. The saying goes “you can sleep when you’re dead.” However, it might be more accurate to say, “if you don’t sleep, you risk death”.
Related Article: 7 Tips To Get You Sleeping Again
You Might Like:
RFK’s Plan to Make America Healthy Again: A Vision for a Healthier Future
Robert F. Kennedy Jr. (RFK Jr.), a prominent environmental lawyer and political activist, has emerged as a voice for change in the United States. Known for his work on environmental and public health issues, particularly...The Science of Temperature Therapy
Temperature therapy (also known as “thermal therapy” or “thermotherapy”) involves the use of heat or cold to improve health and function. Interestingly, thermotherapy has been around for centuries, with ancient cultures regularly using hot springs,...The Predictors of Longevity You Need to Care About
Living a long and healthy life is a universal aspiration, and with the publication of Peter Aittia’s new book “Outlive”, it has never been a bigger focus. With this has come the realisation that, while...How Overtraining and Undertraining Impacts Hormonal Health
While maintaining a healthy hormonal balance is essential for overall health and wellbeing, it is an often-overlooked component of women’s health. Hormones play a vital role in regulating various bodily functions, including metabolism, energy, mood,...12 days of Fitness: 12 Holiday workouts to crush this Christmas
The holiday period is a time for friends, food, and family. With this in mind, it should be a time of guilt-free fun. However, that doesn’t mean you have to neglect your fitness entirely over...Upper Body Strength in Post-Menopausal Women
Menopause is a unique time in the human life, and with it comes a myriad of changes that can have wide reaching health implications. However, over the last 20 years we have seen a strong...References:
Canessa N, Castronovo V, Cappa SF, Aloia MS, Marelli S, Falini A, Alemanno F, Ferini-Strambi L. (2011). Obstructive sleep apnea: brain structural changes and neurocognitive function before and after treatment. Am J Respir Crit Care Med, 183(10):1419-26.
Dempsey JA, Veasey SC, Morgan BJ & O’Donnell CP. (2010) Pathophysiology of Sleep Apnea. Physiol Rev 90(1): 47–112.
Deng W, Aimone JB, Gage FH. (2010). New neurons and new memories: how does adult hippocampal neurogenesis affect learning, memory? Nat Rev Neurosci, 11(5):339-50.
Erickson KI, Voss MW, Prakash RS, Basak C, Szabo A, Chaddock L, Kim JS, Heo S, Alves H, White SM, Wojcicki TR, Mailey E, Vieira VJ, Martin SA, Pence BD, Woods JA, McAuley E,
Kramer AF. (2011). Exercise training increases size of hippocampus, improves memory. PNAS, 108(7):3017-22.
Goldin P, Ziv M, Jazaieri H, Hahn K, Gross JJ. (2013). MBSR vs aerobic exercise in social anxiety: fMRI of emotion regulation of negative self-beliefs. Soc Cogn Affect Neurosci, 8(1):65-72.
Kline CE, Crowley EP, Ewing GB, Burch JB, Blair SN, Durstine JL, Davis JM, & Youngstedt SD. (2011). The effect of Exercise training on obstructive sleep apnea and sleep quality: randomized controlled trial. SLEEP 34(12):1631-1640.
Reid KJ, Baron KG, Lu B, Naylor E, Wolfe L, Zee PC (2010). Aerobic exercise improves self-reported sleep, quality of life in older adults with insomnia. Sleep Med, 11(9):934-40.
Passos GS, Poyares D, Santana MG, Garbuio SA, Tufik S, Mello MT. (2010). Effect of acute physical exercise on patients with chronic primary insomnia. J Clin Sleep Med, 6(3):270-5.
Passos GS, Poyares D, Santana MG, D’Aurea CV, Youngstedt SD, Tufik S, de Mello MT. (2011). Effects of moderate aerobic exercise training on chronic primary insomnia. Sleep Med. 12(10):1018-27.Institute of Medicine. Sleep disorders and sleep deprivation: an unmet public health problem. Washington, DC: National Academies Press; 2006.