Aerobic Exercise – A Treatment For Schizophrenia

Catherine O’Brien
Schizophrenia is a severe and chronic mental disorder that impacts perception, cognition, emotional regulation and thought processes.
According to the National Institute of Mental Health, symptoms of schizophrenia are often categorized as positive, negative, or cognitive. Positive symptoms include hallucinations, delusions, and thought and movement disorders. Negative symptoms include flat affect, reduced feelings in everyday life, poor initiative and persistence and reduced speaking. Cognitive symptoms include impaired executive functioning and trouble with working memory, and difficulty focusing. (National Institute of Mental Health, 2016).
Unlike many other neurodevelopmental disorders, Schizophrenia presents later in life around late adolescence or early adulthood. While the disorder is treatable with antipsychotic medication and therapy, research suggests that introducing a fitness regimen, as a supplement to existing treatment, may improve symptoms of schizophrenia.
Related Article: Improving Cognition Through Exercise
Research conducted by Kimhy, Vakhrusheva et al. (2015) examined the effects of aerobic exercise on physical fitness, neurocognition and levels of brain-derived neurotropic factor (BDNF) in patients with schizophrenia. BDNF is a neurotrophin that supports brain plasticity. It is integral in preservation of existing neurons and the creation of new neurons in the central and peripheral nervous system (NIMH, BDNF). Kimhy et al. pursued this research because prior research regarding the benefits of aerobic exercise suggest patients with schizophrenia may be able to relieve some of their symptoms by adding a physical exercise regimen into their routine.
The Study:
The aim of the study was to understand the effects of aerobic exercise, supplemental to usual treatment, on physical fitness ability, neurocognition and levels of BDNF. Kimhy et al. hypothesized that participants experiencing aerobic exercise would improve in aerobic fitness, neurocognition, and have increased levels of BDNF compared to participants experiencing treatment as usual without the incorporation of aerobic exercise.
Participants in this study were forty-one patients with diagnosed schizophrenia. Upon entry in the study, participants were evaluated with an extensive battery and various clinical assessments. Aerobic fitness was tested using VO2 max which is “an index of the maximum capacity of an individual’s body to transport oxygen during incremental AE (aerobic exercise)” (Kimhy et al. 2015, p860). BDNF samples were collected by way of blood test and centrifugation. MATRICS Consensus Cognitive Battery (MCCB) was used to measure neurocognition. The MCCB includes measures of seven cognitive domains including speed of processing, attention/ vigilance, working memory, verbal learning, visual learning, reasoning, and problem solving, and social cognition.
Related Article: Exercise Increases Neurons in the Brain
Baseline
measurements of diagnostic and clinical tests as well as measures of aerobic fitness, BDNF levels and neurocognition were taken for all participants. There was no significant difference in baseline measurements amongst any of the participants at the start of the study. The same measurements were taken at the conclusion of the 12-week study.
Participants were between ages 18-55 and had not had a medication change in the last 4 weeks. Once eligibility and compliance with criteria were established, participants were randomly divided into two groups.
The first group continued with normal “treatment as usual” (TAU) involving regular doses of antipsychotic medication and therapy visits with psychologists / psychiatrists as well as meetings with social workers and mental health professionals as needed.
Participants in the second group continued TAU but were also prescribed a fitness regimen. This regimen involved 60-minute sessions 3x per week for the course of the 12-week study. Each exercise session consisted of a 10-minute warmup, 45 minutes of aerobic exercise including stationary bicycle, treadmill and elliptical, and 5-minute cool down. Exercise intensity was measured in each session by way of max HR and VO2 max. The goal was to progressively increase intensity starting at 60% of max exertion at the first session and working up to 75%.
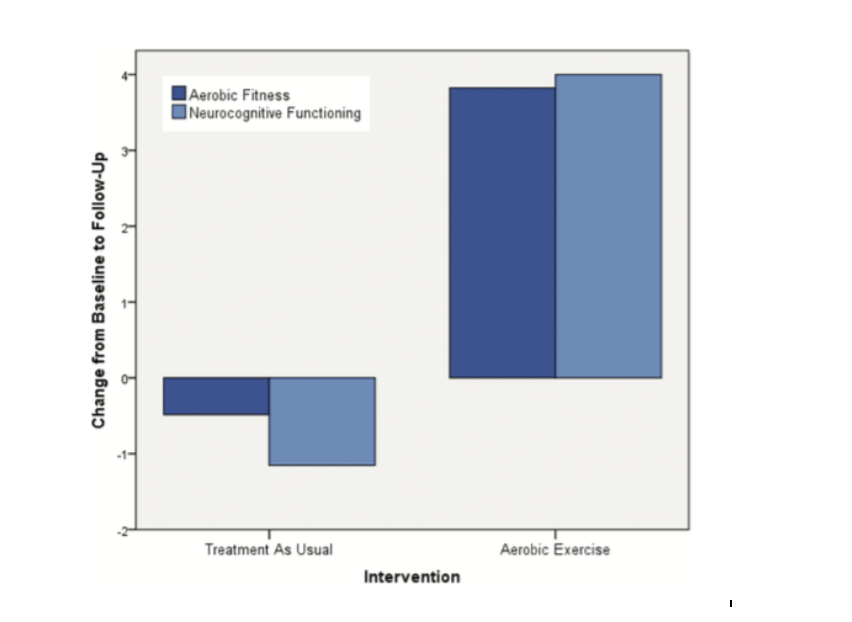
After the 12-week intervention,
improvement in the VO2 max measurement indicated aerobic fitness improved as a result of aerobic training for participants in the exercise condition. The AE group also displayed statistically significant increases in cognitive function compared to the treatment as usual group, according to the MATRICS consensus cognitive battery (See figure below). More specifically, aerobic fitness was correlated to increases in MCCB domains of social cognition and visual learning compared to the TAU group. There was no statistically significant effect in BDNF increase between the two groups.
Related Article: Training Your Body And Brain
Overall,
findings were in line with the predicted results. The aerobic exercise intervention successfully improved some of the key deficits associated with schizophrenia. These findings provide support for the use of exercise as a supplementary prescription for those suffering from schizophrenia. One of the key advantages of supplementing existing treatment programs with exercise is that there are no drawbacks or negative side-effects associated with aerobic exercise. Of course, patients need to be cleared by a physician prior to engaging in physical activity.
References
National Institute of Mental Health (2016). Schizophrenia. Retrieved February 6, 2017, from https://www.nimh.nih.gov/health/topics/schizophrenia/index.shtml.
Kimhy, D., Vakrusheva, J., Brtels, M.N., Armstrong, H.F. et al. (2015) The impact of aerobic exercise on brain-derived neurotrophic factor and neurocognition in individuals with Schizophrenia: A single-blind, randomized clinical trial. Schizophrenia Bulletin, 41(4), 859-868.
You Might Like: